Receiving a cancer diagnosis can be an incredibly challenging time. Many people describe feeling as though their world has been turned upside down — with a loss of control, and a “merry-go-round” of appointments, scans and follow-ups.
Nutrition is one area where you can regain a sense of control. The right support can make a real difference to how confident you feel about food choices during treatment, and how tailored your plan becomes as symptoms, medications and energy levels change.
Cancer nutrition support ranges from a brief “keep your weight up” leaflet at the hospital, to a highly personalised plan that evolves with your treatment and recovery. This guide explains:
what Oncology Dietitian’s typically cover
what My Cancer Nutritionist’s metabolic approach focuses on
how to decide what’s most appropriate for you
Oncology Dietitian vs Oncology Nutritionist: What’s the difference?
What does a Cancer Dietitian do?
Dietitian’s typically work within hospital teams (NHS or private) and are often involved when nutrition becomes clinically complex or urgent.
An oncology dietitian is especially valuable if you need support with things like:
significant unintentional weight loss (especially in a short period of time), and malnutrition risk.
struggling with food intake because of severe nausea, vomiting, pain, Mucositis or swallowing issues
requiring tube feeding or specialised oral nutrition support
stoma support and complex bowel symptoms
In short: dietetic care is crucial when the priority is clinical nutrition management within medical pathways.

Cancer nutrition advice provided by the standard of care medical team is often not personalised, it may include a leaflet or very brief nutrition recommendations. Cancer patients can be advised to:
“Eat whatever you like, just don’t lose weight.”
Other standard of care, cancer nutrition advice may also include suggestions to use energy-dense foods or specific supplemental meal options and shakes designed to prevent malnutrition. Some NHS resources can even include recommending sugary foods, because they are an easy source of calories when appetite is low.
This may feel confusing, particularly if you’re trying to make better, more nourishing choices that support long-term health.
Why hospital nutrition advice can feel generic
The context matters:
Hospital teams are often stretched, and appointments may be brief.
The primary medical concern during active treatment is frequently preventing malnutrition, preserving strength, and reducing complications that can delay treatment.
When someone is barely managing food, the immediate goal can become “anything you can tolerate” rather than a perfect diet.
For some patients, rapid weight and muscle loss is more urgent than dietary optimisation in that moment.
That approach is usually pragmatic and for some patients, the risk of rapid weight and muscle loss is more urgent than dietary optimisation in that moment. Where people often feel underserved is that this approach can’t reflect:
your specific cancer type and treatment plan
your symptoms, your health history or your side effects
your metabolic health (e.g., insulin resistance, diabetes, steroid effects)
your unique physiology, your lab markers, your functional health test results
your preferences, culture, capacity and routine
any guidance on supplements that may be beneficial
That’s where more individualised support can really provide benefit.

What does an oncology nutritionist do, what makes My Cancer Nutritionist’s approach different?
My work is specifically focused on metabolic, personalised cancer nutrition support — designed to sit alongside your medical care. As a BANT Registered Nutritional Therapist, having undertaken highly comprehensive specialist training in cancer care & metabolic health from the Metabolic Terrain Institute of Health as well as with the highly respected Dr Nina Fuller Shavel’s Systems Approach To Cancer Programme, and advanced training in blood testing analysis, my approach is much more in-depth, holistic & personalised than what you may get via a Dietician or standard of care team.
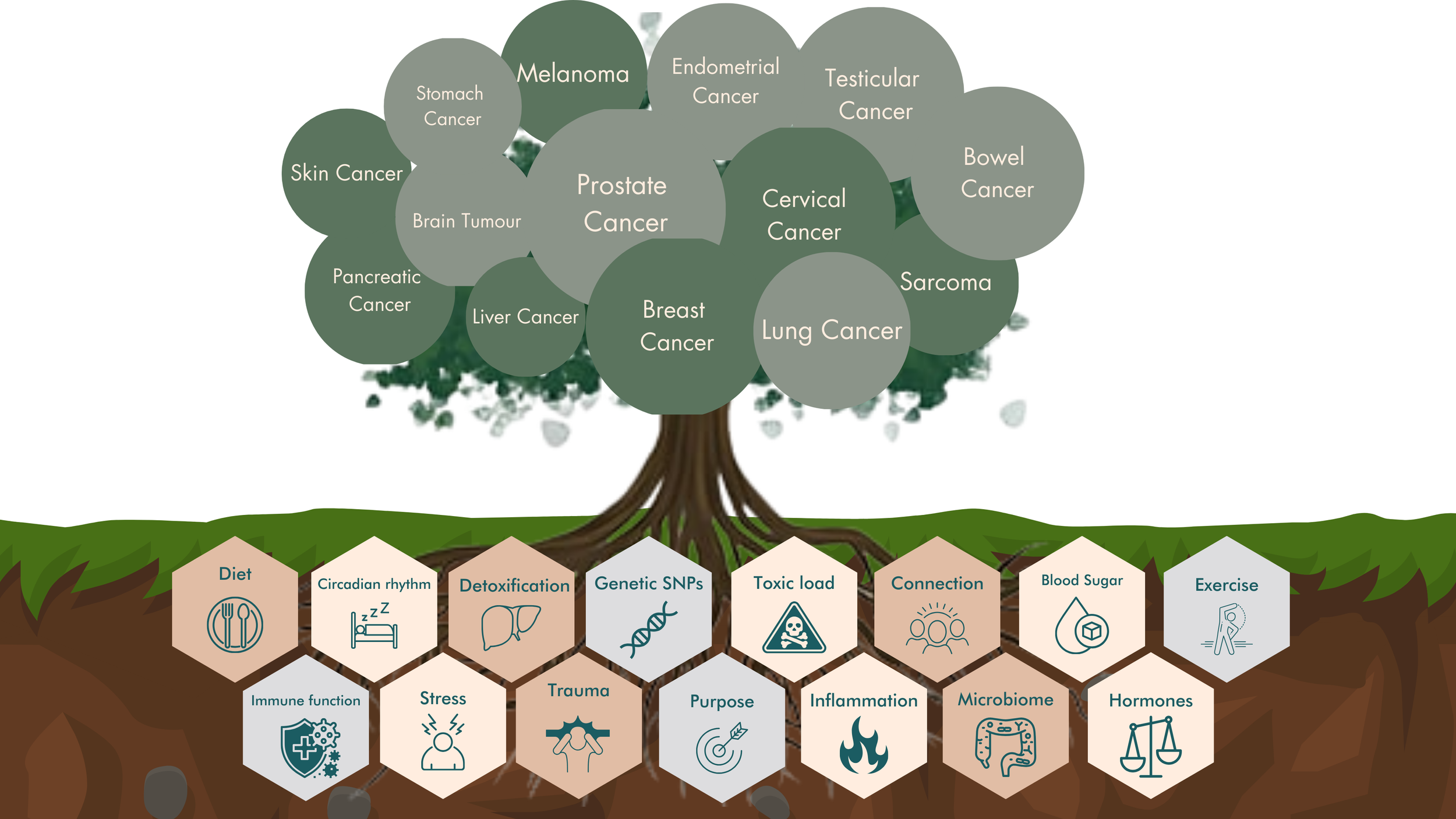
I focus on the terrain that influences how you feel and how well your body copes with treatment and recovery, and investigate the factors that could’ve led you to develop cancer in the first instance. I provide support across:
Blood sugar regulation and metabolic health (using blood tests to measure markers such as Fasting Glucose, Hba1c, Fasting insulin and IGF-1 signalling) and how these may impact on any treatment side effects as well as influence a cancer process. Read more on this topic here.
Inflammation and immune resilience - to support your body as a result of treatment as well as provide targeted nutrition strategies for improving immune system health and reducing inflammation. Testing can also help ascertain the level of inflammation in your body.
Gut terrain and the microbiome, - supporting digestion, nutrient absorption, and microbial diversity. Most of the immune system lives in the gut, but treatment can also impact on the complex bacterial environment even long after treatment finishes - I provide support at all stages.
Nutrient status and how that affects energy, appetite, healing and tolerance. One example of this is essential fatty acid and it’s role in cellular health & immune system health - I offer this as a standalone test -read more about this here.
Sleep, circadian rhythm and stress physiology, because these strongly influence cravings, appetite, blood sugar control and recovery capacity, as well as how well your immune system can fight cancer. Read more about circadian rhythm and cancer here.
Personalised supplement reviews & safety, including interaction checks and what’s appropriate during chemo, radiotherapy, immunotherapy or hormone therapy. Most standard of care don’t provide even basic nutrient testing such as Vitamin D - which is vital for helping fight cancer - read more here.
Hormonal regulation – assessing how hormones influence cancer growth. Functional testing can deep dive into how your body breaks down hormones & whether this requires personalised support.
Genetics & epigenetics – using testing insights to inform personalised nutrition strategies
Detoxification & toxin exposure – optimising pathways to remove harmful compounds and assessing whether there’s a high toxic load or even mould in your body that can contribute to cancer.
Blood Circulation & Angiogenesis - how cancer builds it’s own blood vessels to fuel it’s growth and how targeted nutrition can help.
In short: my role is to create a truly personalised plan that is tailored, realistic, and evolves with you — not just during treatment, but also through recovery and survivorship.
Dieticians may provide dietary guidance and check conventional blood tests for nutrient deficiencies, but they are unlikely to look at you from a functional medicine, root cause perspective, or utilise the many functional tests that I offer which can provide actionable insights into your health.
If you’re losing weight quickly, can’t keep food down, or tube feeding is being discussed, an oncology dietitian is often the most urgent support. If you want a deeper personalised plan that brings together metabolic health, gut support, supplements, sleep/stress and longer-term resilience, that’s the focus of My Cancer Nutritionist. Book a complimentary clarity call to discuss your needs.